Cardiovascular diseases are a leading cause of morbidity and mortality worldwide, with Atherosclerosis standing out as a significant contributor among them. Atherosclerosis is a chronic and progressive condition that affects the arteries, leading to the buildup of plaque and restricting blood flow. This can result in severe health issues if addressed promptly, which is why understanding Atherosclerosis is essential for the prevention and management of the condition.
Atherosclerosis in India
Research has found coronary atherosclerosis is increasing in India. While it is difficult to guage an actual figure of the condition due to under reporting, existing statistics say the prevalence of coronary atherosclerosis is 78% in males and 66.6% in females. Further studies have found how ischemic heart disease and stroke are the predominant causes for >80% of cardio vascular disease deaths in India. Premature mortality in terms of years of life lost because of CVD in India increased by 59%, from 23.2 million (1990) to 37 million (2010). A world health report in 2002 found how 45 million people in India suffer from coronary artery disease with a marked increase among the younger population due to poor lifestyle and food habits.
What is Atherosclerosis?
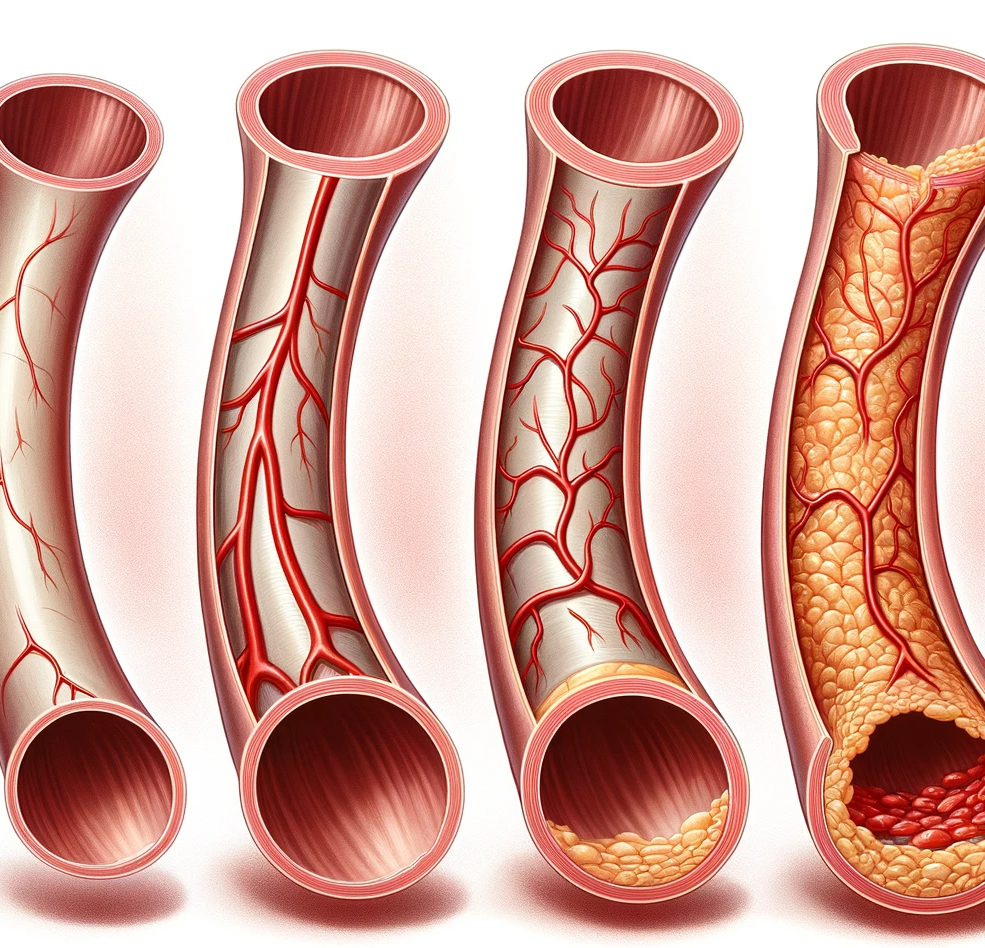
Atherosclerosis is a chronic inflammatory condition involving the accumulation of fatty deposits, cholesterol, calcium, cellular waste, fibrin, and other substances in the inner lining of arteries. This buildup forms plaques, which can gradually narrow, thicken, and harden the arteries, impeding blood flow and supply of oxygen-rich blood to tissues and vital organs. Over time, plaque can rupture, leading to blood clot formation and potentially causing life-threatening complications such as heart attacks and strokes. Atherosclerosis progresses slowly over time and can begin in ages as early as childhood after which it can progress rapidly.
Atherosclerosis begins with damage to the endothelium, the inner lining of arteries. Once the endothelium is compromised, lipids like cholesterol infiltrate the arterial wall, triggering an immune response. Inflammation ensues, leading to the formation of plaques, which may eventually rupture or calcify, further obstructing blood flow.
Causes and Risk Factors
Understanding the causes of Atherosclerosis is essential for prevention and management. Several risk factors contribute to the development of this condition, both modifiable and non-modifiable.
- Unhealthy Diet: Consuming foods high in trans fats, saturated fats, and cholesterol contributes to elevated blood cholesterol levels, fostering plaque formation.
- Physical Inactivity: Lack of physical activity and exercise causes obesity, high blood pressure, and an unhealthy lipid profile, all risk factors for Atherosclerosis.
- Smoking: Tobacco smoke damages the endothelium, accelerates plaque formation, and increases the risk of blood clotting.
- Excessive Alcohol Consumption: Heavy drinking can elevate blood pressure and contribute to unhealthy lipid levels, exacerbating the progression of Atherosclerosis.
- High Blood Pressure: Hypertension can damage artery walls over time, allowing plaque to build up.
- Metabolic Syndrome: High cholesterol and triglycerides in your blood increase your risk.
- Inflammatory diseases: Conditions like rheumatoid arthritis and psoriasis can irritate your blood vessels, leading to plaque buildup.
- Diabetes: Poorly controlled diabetes can lead to high blood sugar levels, promoting inflammation and accelerating Atherosclerosis.
- Age: Atherosclerosis becomes more prevalent with age, and the risk increases significantly after age 45 for men and 55 for women. Women with endometriosis, polycystic ovary syndrome, gestational diabetes, or preeclampsia during pregnancy are at higher risk of the condition.
- Genetics: A family history of cardiovascular diseases can predispose individuals to Atherosclerosis, highlighting the importance of genetic factors.
Signs and Symptoms
Atherosclerosis often progresses silently, with no noticeable symptoms, until it causes an event like a heart attack or stroke. Understanding the signs and symptoms is the only way to detect them early for necessary treatment and intervention.
Angina: Chest pain or discomfort occurs when the heart muscle receives insufficient blood and oxygen.
Shortness of Breath: Reduced blood flow to the heart can lead to difficulty breathing, especially during physical exertion.
Fatigue: Inadequate blood supply to the body’s organs and tissues can result in persistent fatigue.
Leg Pain: Atherosclerosis in the arteries supplying the legs can cause pain, numbness, and weakness, especially while walking or climbing stairs. These are classic symptoms of peripheral artery disease which go away with rest.
Slurred Speech or Weakness: If Atherosclerosis leads to a stroke, symptoms may include slurred speech, weakness, or paralysis on one side of the body. Moreover, Atherosclerosis can cause cognitive problems with thinking, memory, and numbness on one side of the brain or face. Vision trouble is an early sign of vertebral artery disease. A more severe symptom is transient ischemic attack (TIA), commonly called a mini-stroke.
Pain after meals: Severe pain after eating, diarrhea, and weight loss, symptoms of mesenteric artery ischemia of the intestines.
Erectile dysfunction: ED is an early warning sign indicating a higher risk for Atherosclerosis.
Others: Nausea, cold sweats, dizziness, extreme tiredness, and heart palpitations are all symptoms of coronary artery disease
Diagnosing Atherosclerosis
Early diagnosis is crucial for effective management of Atherosclerosis. Various diagnostic tools and tests help healthcare professionals assess the extent of arterial damage and plaque buildup. Your doctor will check your blood tests, imaging results, and other tests, including your medical and family history.
- Physical examination: A thorough examination, including blood pressure measurement and assessment of cardiovascular risk factors, provides valuable initial information.
- Blood tests: Tests included in a diagnosis of Atherosclerosis are lipid profile for cholesterol levels, lipoproteins for C-reactive protein, triglycerides, blood pressure, blood sugar, and your BMI index to calculate your disease risk.
- Electrocardiogram (ECG or EKG): This test records the heart’s electrical activity and can reveal abnormalities indicative of inadequate blood flow.
- Angiography: X-ray imaging with the injection of a contrast dye allows visualization of blood vessels, helping identify blockages.
- Ultrasound: Doppler ultrasound can assess blood flow and identify areas of narrowing or blockage in the arteries.
- Cardiac MRI (magnetic resonance imaging): Detects tissue damage or problems with blood flow in the heart or coronary arteries. A Cardiac MRI is also read in conjunction with other imaging tests, such as chest X-rays and CT scans, to help the doctor better understand the condition.
- Cardiac positron emission tomography (PET) scanning: A type of nuclear heart scan to assess blood flow through the small blood vessels of the heart. It helps in diagnosing coronary microvascular disease.
- Coronary computed tomography (CT) angiography: Provides detailed images of the blood vessels and arteries to help evaluate plaque composition and distribution.
- Coronary calcium scan: A type of CT scan of your heart that measures the amount of calcium in the walls of your coronary arteries. Calcium buildup, or calcifications, are a sign of Atherosclerosis or CAD.
- Stress test: A stress test measures your heart health and how well it functions during physical stress. Some heart problems are more accessible to identify when your heart works harder to pump blood throughout your body during activity or exercise.
- Ankle-brachial index (ABI) test: Ankle-brachial index (ABI) tests diagnose peripheral artery disease by comparing the blood pressures in your ankle and arm using a blood pressure cuff and USG device.
Treatment
The management of Atherosclerosis involves a multifaceted approach targeting risk factors, symptoms, and complications. Lifestyle modifications, medications, and invasive procedures may be employed based on the severity of the condition.
Lifestyle Changes
Healthy Diet: Adopting a diet rich in fruits, vegetables, whole grains, and lean proteins can help lower cholesterol levels. The DASH diet can help with Atherosclerosis.
Regular Exercise: Engaging in physical activity enhances cardiovascular health, promotes weight management, manages blood pressure, cholesterol, and obesity, and improves overall well-being. Adults should engage in 150 minutes or more per week of moderate physical activity or 75 minutes per week of vigorous physical activity. Consult your doctor before resorting to any intense physical activity.
Lose Weight. Losing 3% to 5% of your current weight helps manage some coronary heart disease risk factors, such as high blood pressure, cholesterol, and diabetes. Aim for a healthy BMI.
Avoid smoking: Quitting smoking halts the progression of Atherosclerosis and reduces the risk of complications. Scientific evidence has proved that nicotine and flavorings found in vaping products may also damage your heart and lungs.
Reduce alcohol intake: Reduce your alcohol intake to 2 drinks or less in a day. Women should drink one drink or less per day.
Manage stress. Managing stress, relaxing, and coping with issues can improve your emotional and physical health.
Adequate sleep: Sleep is necessary to reduce stress and protect your heart. Adults need at least 7 to 8 hours of sleep per day.
Medications
Among medications, statins lower cholesterol levels and help prevent plaque buildup. Cholesterol-lowering medicines, and omega-3 fatty acids, may be prescribed if you are unable to take statins or if statins are ineffective in managing cholesterol and triglycerides.
- ACE inhibitors and beta blockers help lower blood pressure and the heart’s workload.
- Calcium channel blockers lower blood pressure by relaxing blood vessels.
- Metformin helps control plaque buildup if you have diabetes.
- Nitrates, such as nitroglycerin, dilate your coronary arteries and relieve or prevent chest pain from angina.
- Antiplatelet medications like aspirin reduce the risk of blood clots.
- Antihypertensives to control blood pressure are crucial to prevent further artery damage.
- Thrombolytic medicines, or clot busters, might be prescribed to treat blood clots resulting from Atherosclerosis. Such medication should be given as soon as possible.
Invasive Procedures
Angioplasty and Stenting: A catheter inflates a balloon, widening narrowed arteries, and a stent may be placed to keep the artery open.
Coronary Artery Bypass Grafting (CABG): In cases of severe blockages, a surgeon may create a bypass using a vessel from another part of the body.
Percutaneous Coronary Intervention (PCI): Opens narrowed coronary arteries blocked by plaque. A small mesh tube called a stent is usually implanted to prevent the artery from checking again.
Weight-loss surgery: This might reduce inflammation, leading to plaque buildup in people with severe obesity.
Management of Atherosclerosis
Atherosclerosis often begins in childhood and continues developing throughout life. Long-term management focuses on preventing the progression of Atherosclerosis, minimizing complications, and improving overall cardiovascular health. Patients with Atherosclerosis should ensure they get regular check-ups to monitor blood pressure, cholesterol levels, and overall cardiovascular health. Consistent prescription medication use is crucial for controlling risk factors and preventing complications. Ensure healthy lifestyle habits, a balanced diet, regular exercise, and avoid smoking for long-term atherosclerosis management.

If you are having problems with weight management in Bengaluru and wish to get help, then Ensocure Integrated Medicine offers comprehensive home health care plans that include weight management, too. One could also visit the in-house obesity clinic in Bengaluru to help reduce weight through nutritionist advice and counseling.

