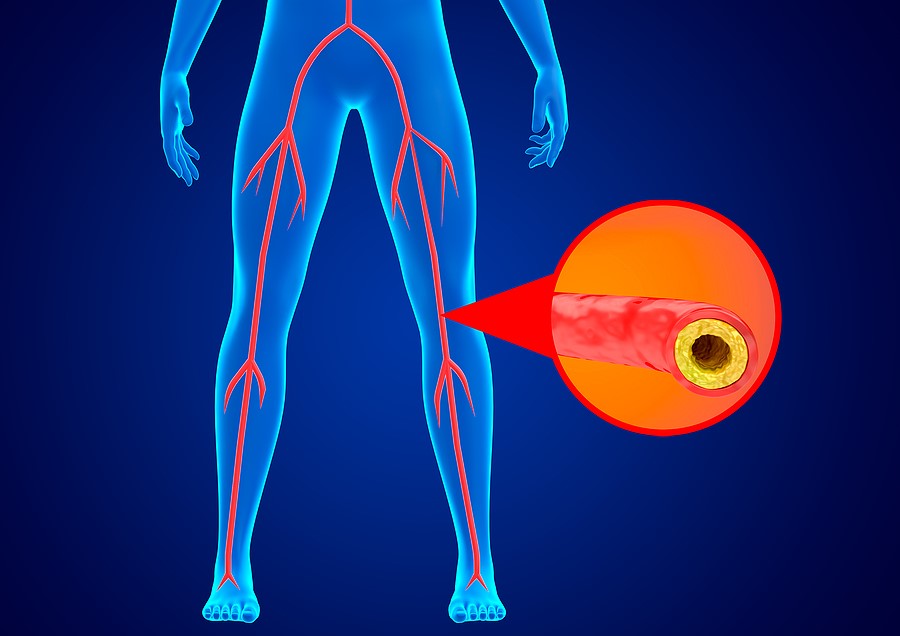
Peripheral Artery Disease is a common health condition characterized by narrowing arteries, which restricts blood flow primarily to the legs and occasionally the arms. This can lead to discomfort, such as leg pain during activities like walking. PAD is often a sign of other underlying health conditions like atherosclerosis. So, understanding its causes, recognizing the symptoms, and getting effective treatments are essential for managing this condition and maintaining a healthy lifestyle.
What is PAD- Peripheral Artery Disease?
Peripheral artery disease (PAD), also known as peripheral arterial disease, is a prevalent condition where the arteries become narrowed, reducing blood flow to the arms or legs. In PAD, most commonly, the legs experience insufficient blood flow. This reduced blood circulation can lead to symptoms like leg pain during walking (claudication). Typically, PAD also indicates a buildup of fatty deposits in the arteries because of atherosclerosis.

PAD shares similarities with coronary artery disease (CAD), as both are caused by atherosclerosis. It is a condition where fatty plaque builds up in arteries, causing blockages throughout the body, including the heart, brain, arms, legs, pelvis, and kidneys.
Causes of Peripheral Artery Disease
The primary cause of PAD is atherosclerosis, characterized by a buildup of fatty, cholesterol-laden plaques on artery walls, reducing blood flow. Atherosclerosis can affect arteries throughout the body, and when it occurs in arteries supplying blood to limbs, it results in PAD.
Other less common causes of PAD include:
- Blood vessel inflammation
- Muscle or ligament changes
- Injuries to arms or legs
- Radiation exposure
Understanding how Atherosclerosis Causes PAD
Atherosclerosis is the accumulation of plaque within arterial walls and is the primary cause of Peripheral Artery Disease (PAD). This plaque consists of fats, cholesterol, and other substances. When plaque builds up in the peripheral arteries, particularly those in the legs, it leads to PAD. Initially, the plaque narrows the artery, reducing blood flow. If this plaque becomes brittle or inflamed and ruptures, it can lead to clot formation, further narrowing or completely blocking the artery.
Blockages in the peripheral arteries of the legs can cause symptoms like leg pain, skin color changes, walking difficulties, and leg or foot ulcers. If it causes total circulation loss, it may result in gangrene or losing a limb. A blockage in a carotid artery can potentially cause a condition called carotid artery stenosis and stroke. This is why understanding PAD is crucial for early diagnosis and management. While PAD often presents common symptoms, some people diagnosed with PAD may not exhibit any symptoms at all. Discussing cardiovascular health with a doctor is vital for those at risk of or diagnosed with PAD.
Risk Factors for PAD
Several factors increase the risk of developing PAD, with smoking and diabetes being major contributors. Other risk factors include:
- Atherosclerosis
- Diabetes
- High blood pressure
- Obesity (BMI over 30)
- Smoking
- High cholesterol levels
- A family medical history of PAD, heart disease, or stroke
- Being above 65 or over 50 with atherosclerosis risk factors
- Increased levels of homocysteine, heightening coronary artery disease risk
While other health conditions can mimic PAD symptoms, it’s important to note that not all PAD cases are due to atherosclerosis. People with PAD are at an increased risk for coronary artery disease and cerebrovascular disease, which can lead to heart attacks or strokes.
Identifying PAD’s Signs and Symptoms
The main symptoms of PAD are leg pain and painful cramps after physical activities like walking or climbing stairs, which typically improve with rest. However, up to 40% of individuals with PAD may experience no leg pain. Peripheral artery disease symptoms may vary, and the severity of pain can range from mild to severe.
Additionally, other symptoms include:
- Claudication in the buttock, hip, thigh, or calf.
- Muscle weakness
- Hair loss or slower hair growth on legs
- Smooth and shiny skin
- Skin color changes
- Skin coolness
- Decreased or absent pulses in the feet
- Cold or numb legs, feet, and toes
- Non-healing leg or foot ulcers
- Arm-use pain
- Slow toenail growth
- Erectile dysfunction
You may also experience pain during rest or when lying down, which may disrupt sleep.
Potential Complications of PAD
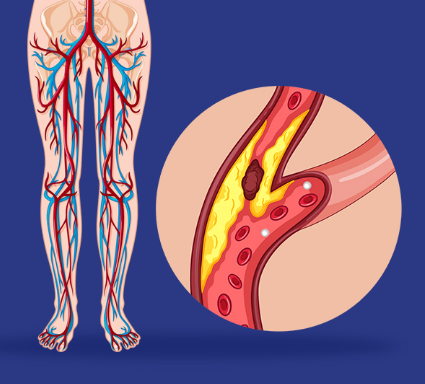
PAD can lead to complications such as critical limb ischemia, where tissue dies due to injury or infection, starting as non-healing open sores on limbs and possibly leading to amputation. Additionally, plaque buildup in arteries can impact blood vessels in the heart and brain, raising the risk of stroke and heart attack.
Diagnosing PAD
For symptomatic individuals, PAD diagnosis may involve an ankle-brachial index (ABI) test, a non-invasive procedure comparing blood pressure in the ankles and arms at rest and post-exercise.
Additional imaging tests may involve:
- Ultrasound
- Magnetic resonance angiography (MRA) or computed tomographic (CT) angiography may also be conducted.
For those at risk or diagnosed with PAD, it’s reassuring to know that PAD can be diagnosed painlessly. Managing PAD may involve adhering to doctor’s recommendations, leading a heart-healthy lifestyle, and, in some cases, medication.
How to Treat and Manage Peripheral Artery Disease (PAD)
Treating and Managing PAD often involves medication and lifestyle changes. Doctors may prescribe aspirin or other antiplatelet medicines to prevent complications arising from PAD and its underlying cause, atherosclerosis. Another common treatment is medication to lower blood cholesterol levels.
Quitting smoking is crucial for individuals with PAD, and doctors can offer assistance and resources to help them quit. In some cases, surgery might be necessary to bypass blocked arteries. Additionally, a supervised exercise program is recommended for those experiencing pain due to reduced blood flow to muscles, aiming to improve functional status and quality of life and alleviate symptoms in the legs.
Prevention Tips for PAD
The most effective way to prevent leg pain and other symptoms associated with PAD is by adopting a healthy lifestyle. The best preventive measures for PAD include:
- Quitting smoking.
- Keeping blood sugar levels under control.
- Eating a diet low in saturated fats.
- Engaging in regular exercise, according to individual needs and capabilities.
- Maintaining a healthy weight.
- Managing blood pressure and cholesterol levels.
- Increasing physical activity to prevent or mitigate PAD symptoms.
- Controlling high blood pressure and preventing or managing diabetes.
For those with PAD, engaging in supervised exercise training programs can significantly enhance and prolong their ability to walk longer distances without discomfort.
Some Quick Facts about Peripheral Arterial Disease
It’s important to note that:
- PAD symptoms are often misinterpreted as other conditions.
- PAD can go undiagnosed by healthcare professionals.
- People with PAD are at increased risk of coronary artery disease, heart attack, and stroke.
- Without treatment, PAD can progress to gangrene and amputation.
Remember to consult your doctor if you are experiencing leg pain, numbness, or other symptoms indicative of PAD. You should promptly seek medical advice from your healthcare provider.