Osteoporosis, often referred to as the “silent disease,” is a condition characterized by weakened bones that are more prone to fractures and breaks. Despite its prevalence and potential severity, many individuals may not be aware of its presence until a fracture occurs. Your bones are living tissue which is constantly regenerating and replaced. However, as you age, this process of building new bone slows down where your body loses bone mineral faster than it can create it. This leads to a decrease in bone putting you at risk of osteoporosis, and brittle and porous bones. Loss of bone density in osteoporosis can be controlled with treatment and exercise.
What is Osteoporosis?
Osteoporosis is a bone disorder characterized by low bone mass and structural deterioration of bone tissue, leading to increased fragility and susceptibility to fractures. While it can affect any bone, fractures commonly occur in the hip, spine, and wrist. The disease is often asymptomatic in its early stages, earning it the moniker “silent disease” as it progresses silently, gradually weakening bones without obvious warning signs.
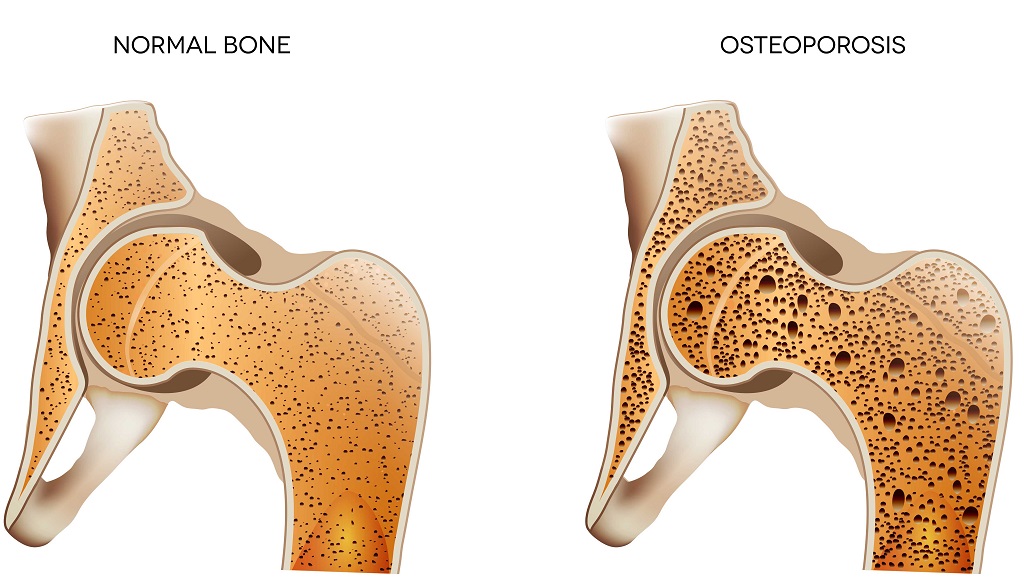
Most people have strong dense bones that support body weight and various impact. But Osteoporosis makes your bones more fragile and weaker losing their absorbing capacity. While the disease is prevalent in old age, sometimes even younger people can be afflicted with the condition. Juvenile osteoporosis can be caused in young children due to an underlying condition that needed intelligent diagnosis by a doctor.
Osteoporosis Prevalence worldwide.
According to research, almost 200 million people suffer from osteoporosis worldwide where 1 in 3 women over the age of 50 years and 1 in 5 men will experience osteoporotic fractures in their lifetime. In India, studies have found how the prevalence of osteoporosis was 18.4, 16.3, 16.4 and 20.7% across east, west, north, and South respectively. 49% were found to have osteopenia, which is a loss of bone mineral density. While not as severe, it can put you at risk of osteoporosis in future.
Signs of Osteoporosis
- Bone Fractures: The most apparent sign of osteoporosis is an increased risk of fractures. Individuals with this condition are more likely to experience fractures from minor falls or even everyday activities, such as bending over or lifting objects. Common fracture sites include the hip, spine, and wrist.
- Loss of Height and Stooped Posture: Osteoporosis can lead to compression fractures in the spine, resulting in a loss of height and a stooped or hunched posture known as kyphosis. This occurs due to the collapse of the vertebral bones in the spine, causing a reduction in overall height.
- Back Pain: As the spine undergoes structural changes, individuals with osteoporosis may experience chronic back pain. This pain is often attributed to vertebral fractures or the compression of nerves in the spine.
- Weakness and Limited Mobility: Weakened bones can contribute to muscle weakness and limited mobility, impacting an individual’s ability to perform daily activities and increasing the risk of falls.
- Shortness of breath (if disks in your spine are compressed enough to reduce your lung capacity).
Causes of Osteoporosis
The main cause of osteoporosis is aging because of the loss of regenerative ability in your bones. However, not everyone in old age will develop osteoporosis, those with a healthier lifestyle, healthy diets and exercise are safeguarded against the condition. There are several things you can do to prevent osteoporosis in old age.
Aging: Advancing age is a primary risk factor for osteoporosis. As individuals age, bone density naturally decreases, making bones more susceptible to fractures. Postmenopausal women are particularly vulnerable due to a decline in estrogen levels, which plays a crucial role in maintaining bone density.
Hormonal Changes: Hormonal imbalances, such as those occurring during menopause or as a result of hormonal disorders, can contribute to bone loss. Estrogen has a protective effect on bone density, and its decline in postmenopausal women can accelerate bone loss.
Family History: Genetics plays a significant role in determining bone health. Individuals with a family history of osteoporosis are at an increased risk of developing the condition. Genetic factors influence bone density, bone structure, and the likelihood of fractures.
Lifestyle Factors:
- Poor Nutrition: Inadequate intake of calcium and vitamin D, essential nutrients for bone health, can contribute to the development of osteoporosis. A diet lacking in these nutrients hinders the body’s ability to build and maintain strong bones.
- Sedentary Lifestyle: Lack of physical activity can lead to decreased bone density. Weight-bearing exercises, such as walking, jogging, and weightlifting, stimulate bone formation and help maintain bone strength.
- Smoking and Excessive Alcohol Consumption: Both smoking and excessive alcohol intake have been linked to an increased risk of osteoporosis. These substances negatively impact bone health by interfering with the body’s ability to absorb calcium and impairing bone formation.
- Medical Conditions and Medications: Certain medical conditions and medications can contribute to the development of osteoporosis. Chronic conditions such as rheumatoid arthritis, celiac disease, and inflammatory bowel disease may affect bone health. Additionally, long-term use of corticosteroids, commonly prescribed for conditions like asthma and arthritis, can lead to bone loss.
Diagnosis of Osteoporosis
Diagnosing osteoporosis involves a combination of clinical assessments, imaging studies, and laboratory tests to evaluate bone density and overall bone health. Here are the key methods used in the diagnosis of osteoporosis.
- Clinical Assessment
- Medical History
- Physical Examination
Bone Mineral Density Test
A trending model of testing bone density is the Dual-Energy X-ray Absorptiometry (DXA). DXA is the most widely used and accurate method for measuring bone density. It uses low-dose X-rays to scan specific bones, usually the spine, hips, or forearm. The results are expressed as a T-score, which compares an individual’s bone density to that of a healthy young adult. A T-score of -2.5 or lower indicates osteoporosis.
Other Tests
- Blood Tests: Blood tests may be performed to measure levels of certain markers related to bone metabolism. For example, tests for calcium, phosphorus, alkaline phosphatase, and vitamin D can provide valuable information about bone health.
- Hormone Levels: Hormonal imbalances can contribute to bone loss. Measuring hormones such as estrogen and testosterone may be relevant, especially in postmenopausal women.
- X-rays: While not as sensitive as DXA for detecting early bone loss, X-rays can identify fractures and assess overall bone health.
- Quantitative Computed Tomography (QCT): QCT is a more advanced imaging technique that can measure bone density and assess the strength of trabecular bone, providing additional information beyond DXA.
- FRAX Tool: The World Health Organization’s Fracture Risk Assessment Tool (FRAX) is an online tool that calculates a person’s 10-year probability of experiencing a major osteoporotic fracture based on various risk factors. It incorporates age, sex, BMI, previous fractures, family history, and other factors.
- Vertebral Fracture Assessment (VFA): VFA is a specialized X-ray imaging technique that focuses on the spine to identify vertebral fractures or assess the structural integrity of vertebrae. It can be performed using the same DXA machine.
Prevention And Management of Osteoporosis
A Healthy Diet
Ensuring a diet rich in calcium and vitamin D is crucial for maintaining bone health. Good dietary sources of calcium include dairy products, leafy green vegetables, and fortified foods. Vitamin D, essential for calcium absorption, can be obtained through sunlight exposure and dietary sources like fatty fish and fortified products.
Regular Exercise
Engaging in weight-bearing exercises, such as walking, jogging, and resistance training, helps stimulate bone formation and strengthens existing bone. Balance and flexibility exercises are also beneficial in reducing the risk of falls.
Lifestyle Modifications
Quitting smoking and moderating alcohol consumption can positively impact bone health. Smoking cessation promotes better circulation, while limiting alcohol intake helps prevent the interference with calcium absorption.
Bone Density Testing
Regular bone density testing, especially for individuals at higher risk, can help identify osteoporosis in its early stages. Early detection allows for timely intervention and management to prevent fractures.
Medication
In some cases, healthcare professionals may prescribe medications to manage osteoporosis and reduce the risk of fractures. These may include bisphosphonates, hormone therapy, or medications that stimulate bone formation.
Osteoporosis is a widespread yet often underestimated condition that can have serious consequences for bone health. By understanding the signs, symptoms, and causes of osteoporosis, you can take proactive steps to prevent its development or manage the condition effectively. Embracing a lifestyle that focuses on good nutrition, regular exercise, and avoidance of harmful habits can contribute to stronger bones and overall well-being.