A healthy bladder is essential for maintaining a healthy lifestyle, but several people tend to overlook certain signals that might suggest bladder problems, like urinary incontinence.
The bladder is an organ that stores urine until it is ready to be eliminated. A healthy bladder can easily hold between 1.5 to 2 cups of urine, but this does not mean you should hold it longer than you should. Urinating helps your body stay healthy, allowing your body to balance fluid loads and rid itself of toxins, and that’s one of the main roles your bladder plays as part of your physiology. Your bladder is also responsible for the sensation that lets you it is full and needs to be voided. In addition, it also helps in motor control to allow you to urinate at will. The most common problem leading to bladder issues, is overactive bladder, and urinary incontinence.
What Is Urinary Incontinence?
Urinary incontinence is a common condition that affects millions of people worldwide. It is characterized by the involuntary leakage of urine, which can be caused by a variety of factors such as age, pregnancy, childbirth, menopause, obesity, and certain medical conditions. While it can be an embarrassing and uncomfortable condition, there are several ways to manage and prevent urinary incontinence.

Besides weak pelvic floor muscles, urinary incontinence can be caused by urinary tract infections which is accumulated bacteria in the urinary tract. These infections can irritate the bladder and can lead to chronic or temporary incontinence, in extreme cases, pain. Moreover, a weak bladder can also be the cause of neurological conditions like neurogenic bladder neurological disease and issues like stroke, multiple sclerosis, spinal cord injury, or spina bifida break down communication between the bladder and the brain. Besides medical conditions, muscle Relaxants, diuretics, sedatives, and other types of medications can also have an impact on bladder control eventually leading to incontinence.
What Happens in Normal Functioning Bladder?
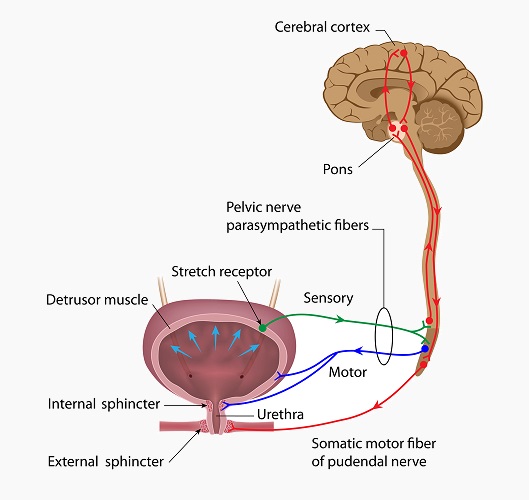
Your brain plays a crucial role in controlling the bladder and the process of urination. Neural circuits extending from the cerebral cortex to the bladder maintain urinary continence and allow voiding when it is socially appropriate. When your bladder is full, it signals the brain which relay back the message it’s ok for you to pee. The brain also controls the muscles that help the bladder empty completely. Injuries to certain brain regions can produce a specific disruption known as urge incontinence, which is characterized by bladder spasticity, with sudden urges to void and frequent inability to maintain continence. Identifying the specific cell types and circuit connections that constitute the continence-promoting pathway, from the forebrain to the brainstem, helps researchers better understand why some brain lesions and neurodegenerative diseases disrupt continence. The information is crucial in paving the way toward better treatments for neurologic patients suffering from urge incontinence.
Types of Incontinence
Urinary incontinence can be classified into 3 types and it is necessary to identify the symptoms as early as possible for finding the plausible solution. The initial stages of urinary incontinence are:
Stress Incontinence: This occurs when there is increased pressure on the bladder, leading to leakage of urine. Activities such as coughing, sneezing, laughing, or heavy lifting can trigger stress incontinence. Weakness of the pelvic floor muscles, which support the bladder and urethra, is a common cause. The issue is usually related to weak pelvic floor muscles which is caused by pregnancy, hormonal changes, or childbirth. There are different types of incontinence.
Urge incontinence: Also known as overactive bladder, urge incontinence is characterized by a sudden and intense urge to urinate, followed by an involuntary loss of urine. The bladder muscle contracts inappropriately, causing this urge. This is caused by involuntary contraction of bladder muscles which leads to frequent urination. Bladder infections, neurological disorders and other types of medications can cause this condition. Some research has even found how thyroid imbalance like Hashimoto’s can impact the bladder making it difficult to pass urine and promote urgency and incontinence.
Overflow Incontinence: This occurs when the bladder is unable to empty properly, leading to a constant dribbling of urine. It often happens when the bladder muscles don’t contract effectively, and it can be caused by conditions like an enlarged prostate in men, nerve damage, or urinary tract obstructions. Overflow incontinence can even be caused by nerve damage, urinary stones or enlarged prostate.
Functional incontinence: This type is not directly related to problems with the bladder or urinary tract but is due to other factors such as physical or cognitive impairments that make it difficult for a person to reach the toilet in time.
Mixed incontinence: Some individuals may experience a combination of two or more types of incontinence. For example, a person may have both stress and urge incontinence.
Diagnosis
Diagnosing urinary incontinence involves a thorough evaluation by a healthcare professional. The process typically includes a detailed medical history, physical examination, and sometimes additional diagnostic tests. It’s important to determine the type of urinary incontinence that you have, and your symptoms often tell your doctor which type you have to propose an accurate treatment plan.
- Medical History: The healthcare provider will inquire about the patient’s symptoms, including the type and frequency of incontinence, any triggering factors or patterns, and the duration of symptoms. Information about the patient’s medical history, medications, lifestyle, and any relevant surgeries or treatments is crucial for understanding potential contributing factors.
- Physical Examination: A physical examination, including a pelvic examination for women and a genital and rectal examination for men, may be conducted to assess the pelvic floor muscles and the condition of the urinary and reproductive organs. Neurological examinations may be performed to identify any signs of nerve damage or dysfunction.
- Urinalysis: A sample of your urine is checked for signs of infection, traces of blood or other abnormalities.
- Bladder diary: Keeping a bladder diary involves recording details such as fluid intake, urination frequency, episodes of incontinence, and any associated factors (e.g., activities, foods, or drinks that may exacerbate symptoms). This can provide valuable information about patterns and triggers.
- Postvoid residual measurement: PVR measurement assesses how much urine remains in the bladder after voiding. Then your doctor checks the amount of leftover urine in your bladder using a catheter or ultrasound test. High residual volumes may indicate an issue with bladder emptying.
- If your doctor feels you might need surgery, then further tests are required such as:
- Urodynamic Testing: Urodynamic tests assess how well the bladder, sphincters, and urethra are storing and releasing urine. These tests can include cystometry, pressure flow studies, and electromyography (EMG).
- Imaging Studies: Imaging tests, such as ultrasound or cystoscopy, may be used to visualize the urinary tract and identify any structural abnormalities, tumors, or obstructions.
- Blood Tests: Blood tests may be conducted to check for underlying medical conditions or assess kidney function.
READ: Tips on Travelling with an Overactive Bladder
Treatment for urinary incontinence depends on the type and underlying cause. It can include lifestyle modifications, pelvic floor exercises, medications, medical devices, or, in some cases, surgery. It’s important for individuals experiencing symptoms of urinary incontinence to consult with a healthcare professional for a proper diagnosis and appropriate management. Here are some of the most common treatments:
Behavioral techniques and Lifestyle Interventions:
- Pelvic Floor Exercises (Kegel exercises): Strengthening the pelvic floor muscles can help improve bladder control.
- Bladder Training: Gradually increasing the time between bathroom visits and scheduling regular, timed voiding.
- Fluid Management: Adjusting fluid intake, particularly avoiding caffeine, alcohol, and can help reduce symptoms. Caffeine is a known diuretic which may increase the urge to void.
- Weight Management: Losing excess weight can reduce pressure on the bladder and improve symptoms.
- Dietary Changes: Avoiding bladder irritants such as caffeine, spicy foods, and acidic foods may help.
- Management of Underlying Conditions: Treating any underlying medical conditions contributing to incontinence, such as urinary tract infections or constipation.
Medications
Certain medications like anticholinergics, Beta-3 Agonists, and alpha blockers can help relax the bladder muscles and prevent involuntary contractions that cause urinary incontinence.
Nerve Stimulation
Nerve stimulation helps control the nerves and attempts to change the messaging to the bladder. Small electrical pulses are sent to the nerve through a needle to decrease urge symptoms temporarily. Sacral nerve stimulation is suggested as a last resort in severe incontinence. This employs a device surgically implanted near the spine with a battery surgically implanted into the buttocks area.
Topical Estrogen Therapy
In postmenopausal women, topical estrogen may be prescribed to improve the tone and elasticity of the urethra and vaginal tissues.
Medical devices
Medical devices such as urethral inserts, pessaries, and catheters can help manage urinary incontinence in some cases.
Surgery
Surgery may be recommended for severe cases of urinary incontinence that do not respond to other treatments. Surgical options include sling procedures, bladder neck suspension, and artificial urinary sphincter
Read: Tips for a Healthy Bladder
Treatment for urinary incontinence depends on the type and underlying cause. There are several issues which may be causing your urinary incontinence which is why its always best never to treat yourself, but at the same time never void addressing it either. Always consult your doctor or a urologist for an accurate diagnosis and treatment.

