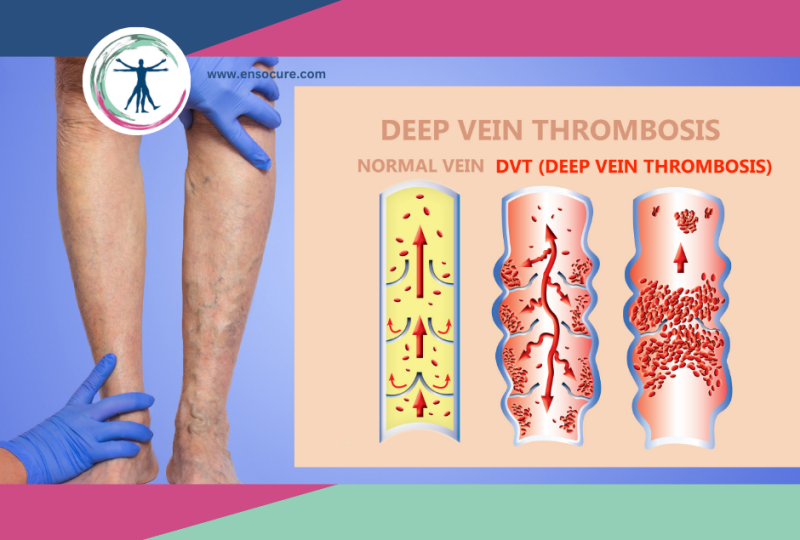
Deep Vein Thrombosis or (DVT) is a condition characterized by the formation of blood clots in deep veins, typically in the legs. While often asymptomatic, DVT can lead to severe complications such as pulmonary embolism if left untreated. DVT needs to be nipped in the bud early through understanding its symptoms, and diagnosing is soon enough to start treatment and management which is crucial for preventing life-threatening consequences.
What is Deep Vein Thrombosis
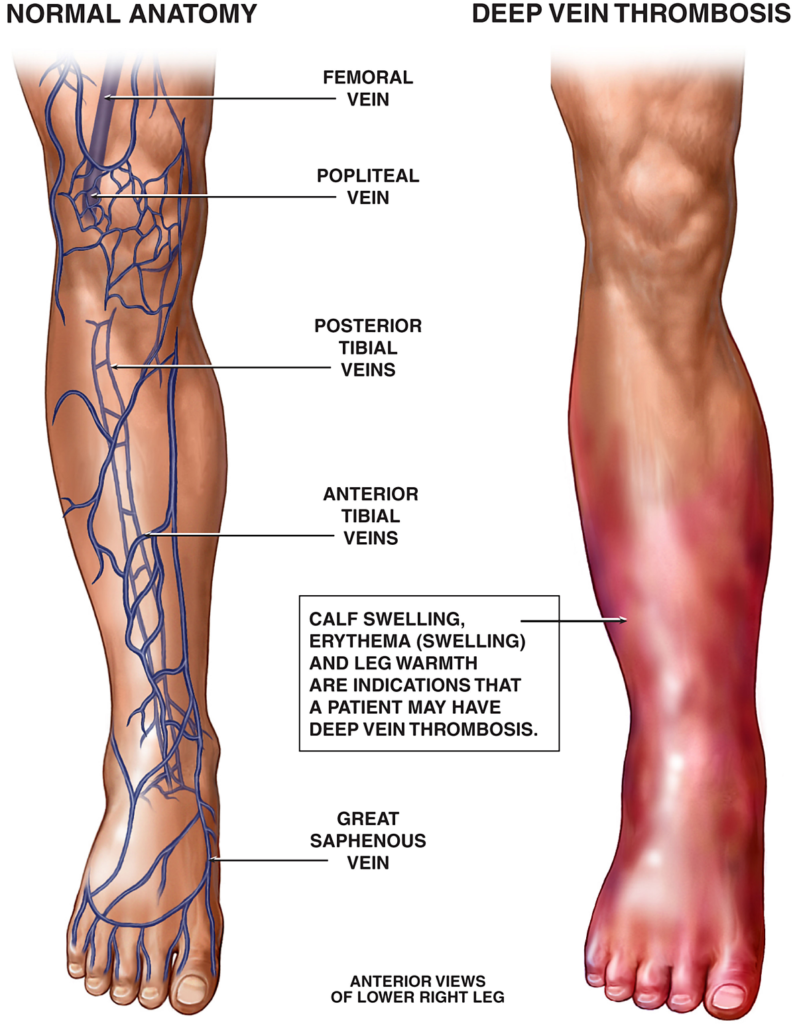
The human body has three types of veins that contribute to the circulatory system. These are:
- Superficial Veins: Located close to the surface of the skin and responsible for draining blood from the skin and superficial tissues. They are often used for medical procedures such as venipuncture and intravenous therapy. Examples of superficial veins include the cephalic vein in the forearm and the great saphenous vein in the leg.
- Deep Veins: Deep veins are located deeper within the body and are surrounded by muscles and tissues. These carry most of the blood volume back to the heart from the body’s organs and tissues. Deep veins typically travel alongside arteries and are less visible from the surface of the skin compared to superficial veins. Examples of deep veins include the femoral vein in the thigh and the popliteal vein behind the knee.
- Perforating Veins (Communicating Veins): Perforating veins connect the superficial veins to the deep veins and help regulate blood flow between the two systems. These veins contain one-way valves that prevent the backward flow of blood and ensure that blood moves efficiently toward the heart. Perforating veins are essential for maintaining proper circulation and preventing conditions such as chronic venous insufficiency. Examples of perforating veins include the Cockett veins in the leg and the Boyd veins in the forearm.
Each type of vein plays a vital role in the circulatory system, working together to ensure that oxygenated blood is delivered to the body’s tissues and deoxygenated blood is returned to the heart for reoxygenation.
Deep vein Thrombosis is a blood clot that forms within one or more of the deep veins usually in the leg. If not treated in time, it can break free from its location and travel up to the lungs where the condition is known as Pulmonary Embolism. Both DVT and PE go hand in hand. Unchecked, DVT ultimately causes stroke, heart attack and death. Venous thromboembolism (VTE) refers to DVT, PE, or both.
According to studies, Venous thrombosis, comprising deep vein thrombosis (DVT) and pulmonary embolism (PE) affects 1 in every 1000 people worldwide. In India, the prevalence is 1.79 per 1000 population. Approximately 30 % of patients with symptomatic VTE display signs of PE, and others with DVT. What are the major factors contributing to such an alarming trend of DVT. Only awareness and prevention of the contributing factors of DVT and PE can help people reduce this calamity that is slowly increasing with every passing year
Causes of Blood Clots in Legs leading to deep vein Thrombosis
Deep Vein Thrombosis in Legs can be caused by any condition or event that results in the damage of blood vessels, hypercoagulability (Increased tendency of blood clotting) or changes in blood circulation. The largest possible factors contributing to such conditions are:
- Immobility or sitting for long periods of time
- Prolonged bed rest during illness or recovery
- Recent orthopedic surgery
- Obesity
- Pregnancy
- Heart attacks and cardiovascular disease
- High altitudes such as 14000 feet
- Undergoing estrogen therapy and birth control pills
- Old age
- Venous problems such as varicose veins and vasculitis
- Smoking
- Legs fractures and severe bruises
- Invasive procedures affecting veins
- Irritable bowel syndrome
- Lung problems
- Increased RBC count
- Increased coagulation of blood
How Blood Clots Lead To DVT
If blood clots formed in deep veins remain stationary, they may not be fatal. Blood clotting is a natural process of the body’s preventive measures for healing wounds and injuries. Without such a condition, we would all bleed to death from a single wound where the condition is known hemophilia or the inability of blood clotting. It is when blood clots where it isn’t supposed to which causes Deep Vein Thrombosis. The most common areas for DVT to occur are the lower extremities like the thighs, calves and thighs.
Symptoms of Deep vein thrombosis?
In DVT, inflamed blood clots cause noticeable symptoms such as
- A warm feeling around the calves or inflamed area
- Redness surrounding the clot
- Tenderness
- Swelling of feet and areas below the calves
- Leg pain when bending feet
- Frequent muscle cramps especially in the calf area
- Discoloration of skin to white or blue tints
- Sudden appearance of varicose veins
In several instances of deep vein thrombosis, the veins can bulge and look like a thick piece of cord. Old age is one condition where rigidity causes veins to stretch. Valves usually fail which causes a vein to swell and appear distorted. Deep vein Thrombosis has also been known to be confused with common cellulitis or common infections. Regardless of such, whenever there is a sudden swelling in the feet or legs, a doctor should be consulted immediately.
Common causes of asymmetric leg swelling that mimic DVT:
- Soft-tissue trauma
- Cellulitis
- Compression of a pelvic vein
- Obstruction of a lymphatic vessel in the pelvis
- Popliteal cyst (Baker cyst) that obstructs venous return
Deep Vein Thrombosis and Pulmonary Embolism
When Deep vein Thrombosis is undetected or neglected, it leads to pulmonary Embolism a fatal complication of DVT. The condition can have serious and fatal consequences. Pieces of blood clots that are allowed to grow can break off and travel to the lungs where it obstructs blood flow thereby reducing oxygen distribution throughout the body.
Symptoms of Pulmonary Embolism
- Excessive sweating
- Sharp chest pains
- Increased pulse rates
- Breathing difficulty
- Blood in sputum
- Dizziness and fainting
Early detection and treatment of DVT can reduce or even prevent the risk of Pulmonary Embolism. Prompt diagnosis of DVT is essential for effective treatment and prevention of complications. Diagnostic methods include:
Ultrasound: Doppler ultrasound is the primary diagnostic tool for DVT. It uses sound waves to create images of blood flow in the veins, allowing healthcare providers to detect blood clots.
D-dimer Test: A D-dimer blood test measures the levels of a substance released when blood clots break down. Elevated D-dimer levels may indicate the presence of a blood clot, although this test is not specific to DVT and may require further evaluation.
Venography: Venography involves injecting a contrast dye into a vein and taking X-ray images to visualize blood flow and detect blockages.
In such cases medical blood thinners such as Heparin or Coumadin are used for reducing the tendency for hypercoagulation or increased blood clotting. DVT is diagnosed through a regular USG (ultrasonography) and a D-Dimer test which determines the presence of blood clots in the body.
Complications of Deep Vein Thrombosis?
Besides PE, deep Vein thrombosis can also lead to Post Phlebetic syndrome where the infected part of the leg is discolored permanently. Ulcers also begin to form around the ankles. Patients unable to consume blood thinners then need to undergo invasive procedures as a last resort of treatment for deep vein thrombosis. The procedure involves placing an inferior Vena Cava into the infected area that acts as a filter for preventing recurring and future blood clots from infecting the lung.
Treatment for Deep Vein Thrombosis
Treatment for DVT aims to prevent the clot from growing larger, reduce the risk of pulmonary embolism, and prevent recurrence. Common treatment options include:
- Anticoagulant Medications: Anticoagulants, or blood thinners, are the primary treatment for DVT. These medications prevent new clots from forming and help existing clots from getting bigger. Commonly prescribed anticoagulants in India include heparin, warfarin, Parnaparin, and phenindione.
- Thrombolytic Therapy: Thrombolytic therapy, also known as clot-busting therapy, involves the administration of medications such as tissue plasminogen activator (tPA) to dissolve blood clots quickly. This treatment is typically reserved for severe cases of DVT or when there is a high risk of pulmonary embolism.
- Compression Stockings: Compression stockings help prevent blood from pooling in the legs and reduce the risk of DVT recurrence. These specialized socks apply gentle pressure to the legs, promoting blood flow towards the heart.
- Inferior Vena Cava (IVC) Filters: In rare cases where anticoagulant therapy is contraindicated or ineffective, an IVC filter may be inserted into the inferior vena cava to trap blood clots and prevent them from traveling to the lungs.
Management of Deep Vein Thrombosis:
In addition to medical treatment, lifestyle modifications and self-care measures can help manage DVT and reduce the risk of recurrence:
Stay Active: Engaging in regular physical activity, such as walking or swimming, promotes blood circulation and reduces the risk of blood clots.
Maintain a Healthy Weight: Losing excess weight can reduce pressure on veins and lower the risk of DVT.
Elevate Legs: Elevating the legs above heart level when sitting or lying down helps reduce swelling and improve blood flow.
Avoid Prolonged Immobility: Take frequent breaks during long periods of sitting or standing to stretch and move around.
Follow Medication Instructions: Take anticoagulant medications as prescribed by healthcare providers and attend regular follow-up appointments for monitoring.
How to prevent Deep Vein Thrombosis
- Annual medical checkups
- Avoid misconceptions of blood thinners and intake of vitamin K by consulting your doctor
- Move around more often after surgery or prolonged illness
- Don’t sit in one place for prolonged periods. Move around at intervals
- Use compression stockings for improving blood circulation during hospital confinement
- Exercise regularly where walking is fine
- Lose weight if obese or even overweight
- Stop smoking
- Perform heel toe exercise when immobile
- Drink plenty of water
- Remain active
- Consult your doctors for the implications of blood clotting when on hormonal therapy
Remember, Deep vein thrombosis is a serious condition. You need prompt diagnosis and treatment to prevent it progressing into a life-threatening situation. Adopting healthy lifestyle habits are the best way to protect your cardiovascular health and reduce the risk of DVT.